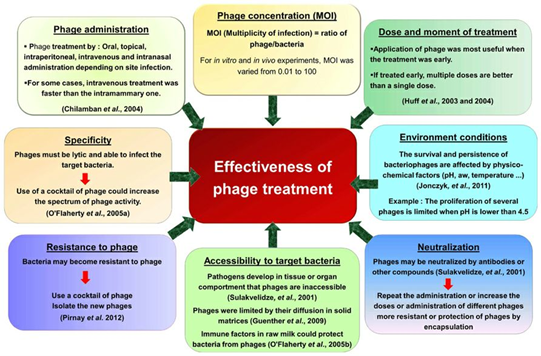
Phage therapy
Phage therapy is a promising approach for treating antibiotic resistant bacterial infections. As there is no remedy for everything, several limitations also restrict its large scale application, which include the specificity of phage host range, the resistance of the bacteria, and the manufacturing procedures of phage products. Thus, the continuous and collaborating efforts in phage biology are crucial in providing insights in designing improved phage therapy strategies. Bacteriophages offer an alternative for the treatment of multidrug-resistant bacterial diseases as their mechanism of action differs from that of antibiotics. However, their application in the clinical field is limited to specific cases of patients with few or no other alternative therapies. Likewise, the discovery and development of new antibiotics have decreased because of the large amount of time and money required, resulting in increasingly difficult clinical management of infections and, in some cases, infections that are impossible to treat. For these reasons, there is a need to look for alternatives for patients for whom conventional antibiotic therapy is ineffective. Thus, phage therapy has become an alternative as its mechanism of action differs from that of antibiotics. Lytic bacteriophages have had an impact on the clinical treatment of multidrug- resistant bacteria because of their capacity to naturally control bacterial populations. These viruses provide novel advantages, such as the safe treatment of infections, as they are harmless to eukaryotic cells, do not cause harmful side effects, and demonstrate high host specificity. This is because they only replicate in the presence of bacteria causing the infection, thus reducing damage to the natural microflora. In addition, genetic exchange between phages rarely happens. Therefore, as the frequency of therapy increases, the treatment doses and periods needed to achieve an optimal effect are expected to decrease. Phage therapy has been used for the treatment of infections related to burn injuries or soft tissue and skin trauma, osteomyelitis, sepsis, bacteremia, and otitis media as well as urinary tract, pulmonary, and prosthetic device-associated infections. It is often used after the generally prolonged stay of the patients, who have been treated with different antibiotics without being able to eradicate the infection successfully. However, effectiveness- and safety-related data for this type of therapy are scattered across individual clinical case reports owing to the few clinical studies conducted<br /><br />MSc Ata'a Khalil Hussein