Millimetric Precision: How Radio-Physics Engineers Cancer Treatment Plans
26/03/2026 Share :
In modern academic and medical circles, physics is no longer just a collection of theoretical equations; it has evolved into a practical tool embodying "Bio-Engineering" to directly save lives. Clinical Radio-Physics stands as a fundamental pillar in designing and executing cancer treatment plans, balancing the eradication of malignant cells with the preservation of healthy tissues.
1. From Theory to Bedside: Complex Computational Language
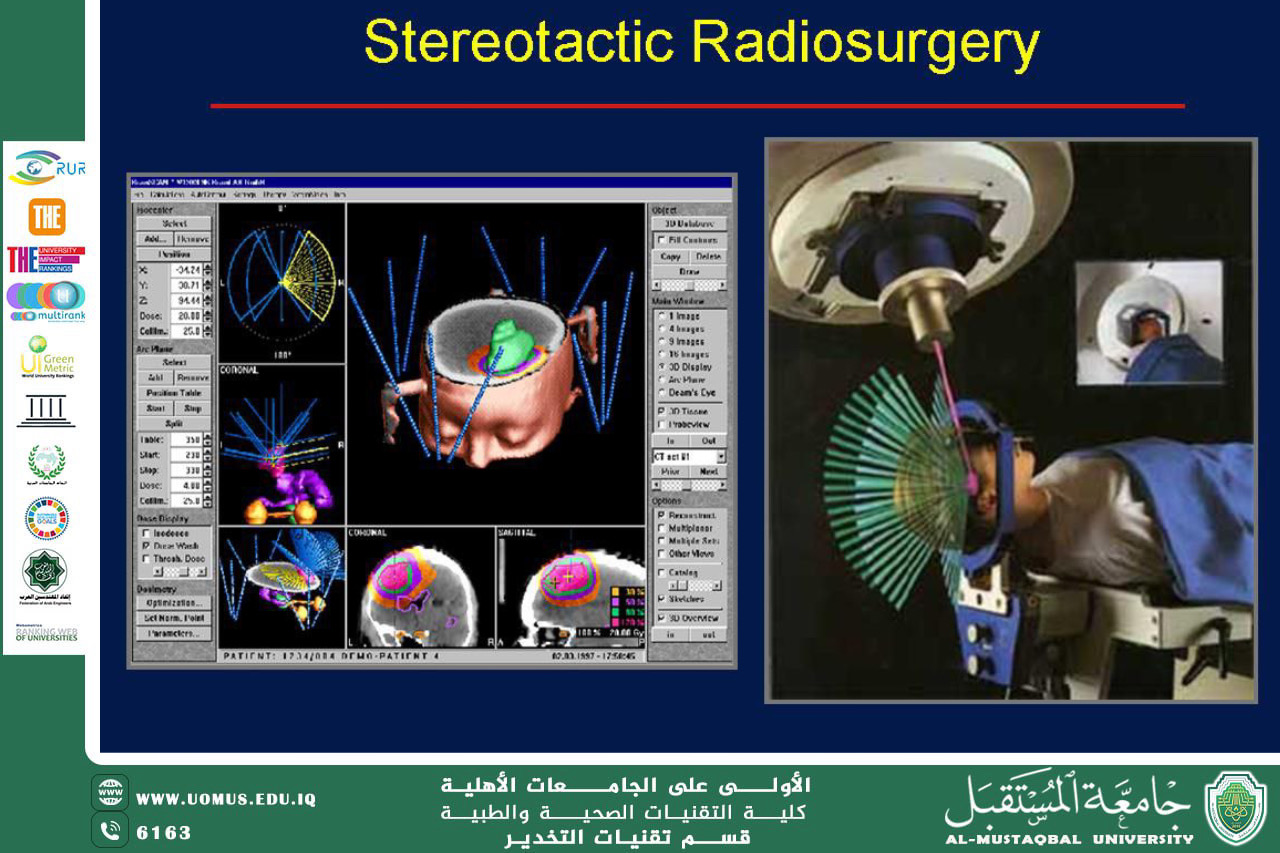
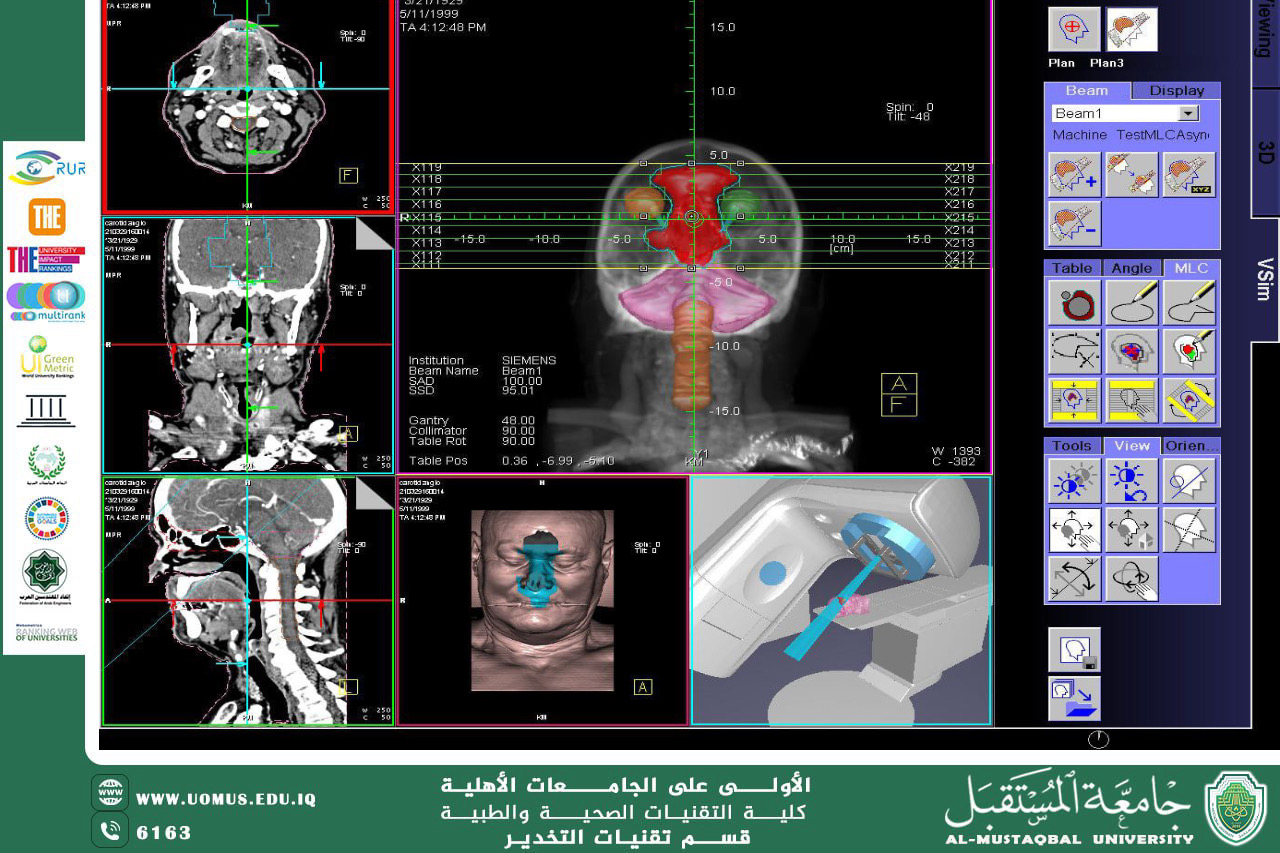
The patient’s journey begins at the CT-Simulator and concludes at the Linear Accelerator (LINAC). Between these two stages, Dosimetry plays a pivotal role.
• Advanced Algorithms:
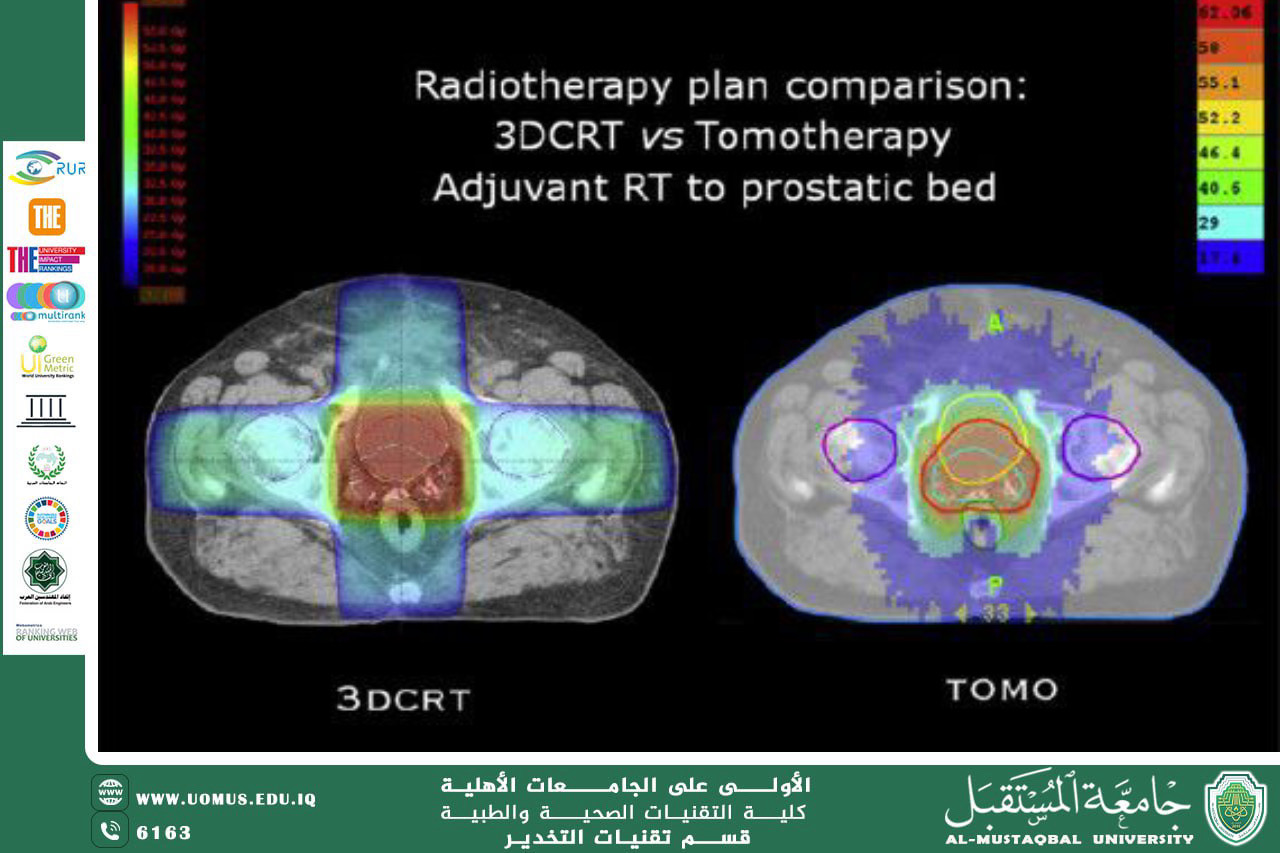
Sophisticated algorithms, such as Monte Carlo simulations, are used to model the paths of millions of photons within the body. These calculations account for density variations between bone, lung, and soft tissues, ensuring precise radiation dose distribution.
• Volumetric Modulated Arc Therapy (VMAT):
This technique relies on the machine rotating 360^{\circ} around the patient. This allows the radiation dose to be concentrated within the tumor while significantly reducing exposure to the surrounding healthy tissues.
2. Control Engineering: Mapping Safety Zones
To ensure accurate tumor targeting, a set of physical volumes is defined according to strict criteria:
• GTV (Gross Tumor Volume): Represents the visible mass of the tumor in radiographic images.
• CTV (Clinical Target Volume): Includes areas potentially containing microscopic cancer cells.
• PTV (Planning Target Volume): A safety margin added to compensate for patient movement or respiration.
- Physical Rule: The higher the precision of radiographic imaging, the smaller the PTV margin can be, leading to better protection of healthy tissues and fewer side effects.
•
3. Motion Tracking (Gating): Real-Time Execution Precision
Moving tumors (such as those in the lungs or liver) pose a significant challenge due to respiratory motion.
Respiratory Gating technology relies on:
• Linking the radiation device to sensors that monitor chest movement.
• Triggering the radiation beam only when the tumor reaches a specific position within the respiratory cycle.
This ensures millimetric therapeutic precision in targeting the tumor.
4. Clinical Quality Assurance (QA): The Safety Valve
Before treatment commences, rigorous tests are performed to ensure the accuracy of the plan using a Phantom (a device that mimics the physical properties of human tissue).
• Verification Steps:
• Comparing the computer-calculated dose with the dose actually measured.
• Using high-precision sensors inside the phantom to simulate real-world conditions.
• Global Standard:
The coincidence rate must exceed 95% to ensure the safety and efficacy of the treatment plan before it is applied to the patient.
: Conclusion
Clinical Radio-Physics represents the intersection of science and humanitarian application, striving to achieve a delicate equation: Maximum destruction of cancer cells versus minimum possible damage to healthy tissues.
Zahraa Jawad
Al-Mustaqbal University
The First University in Iraq