Radiation Therapy and Radiation Protection Scientific Article by Msc. Ali Salman titled:
01/04/2026 Share :
Introduction
Cancer is one of the most significant health challenges of the modern era. Its treatment relies on multiple approaches, including surgery, chemotherapy, and radiation therapy. Radiation therapy is considered one of the main pillars in cancer treatment, being used in more than half of all cancer cases. This treatment modality depends on the use of ionizing radiation to destroy cancer cells while preserving healthy tissues as much as possible.
Principle of Radiation Therapy
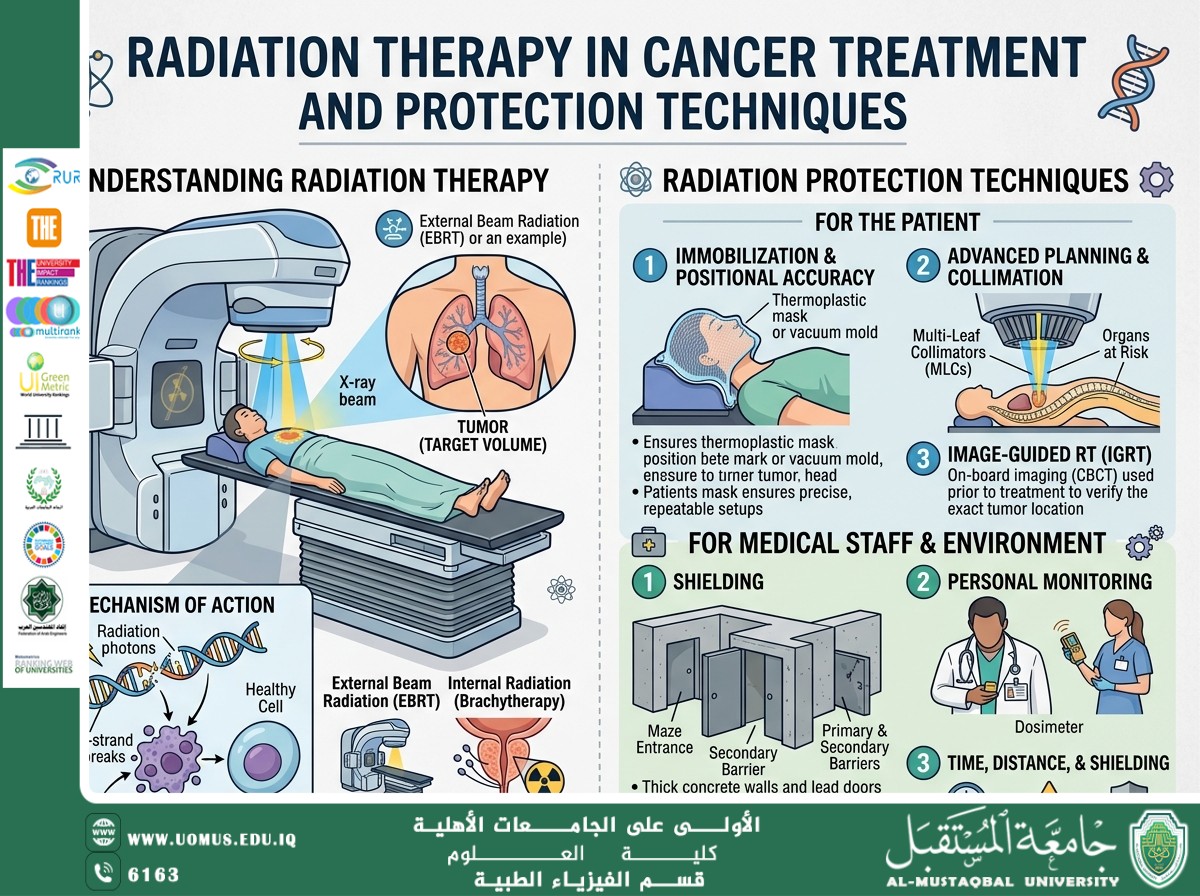
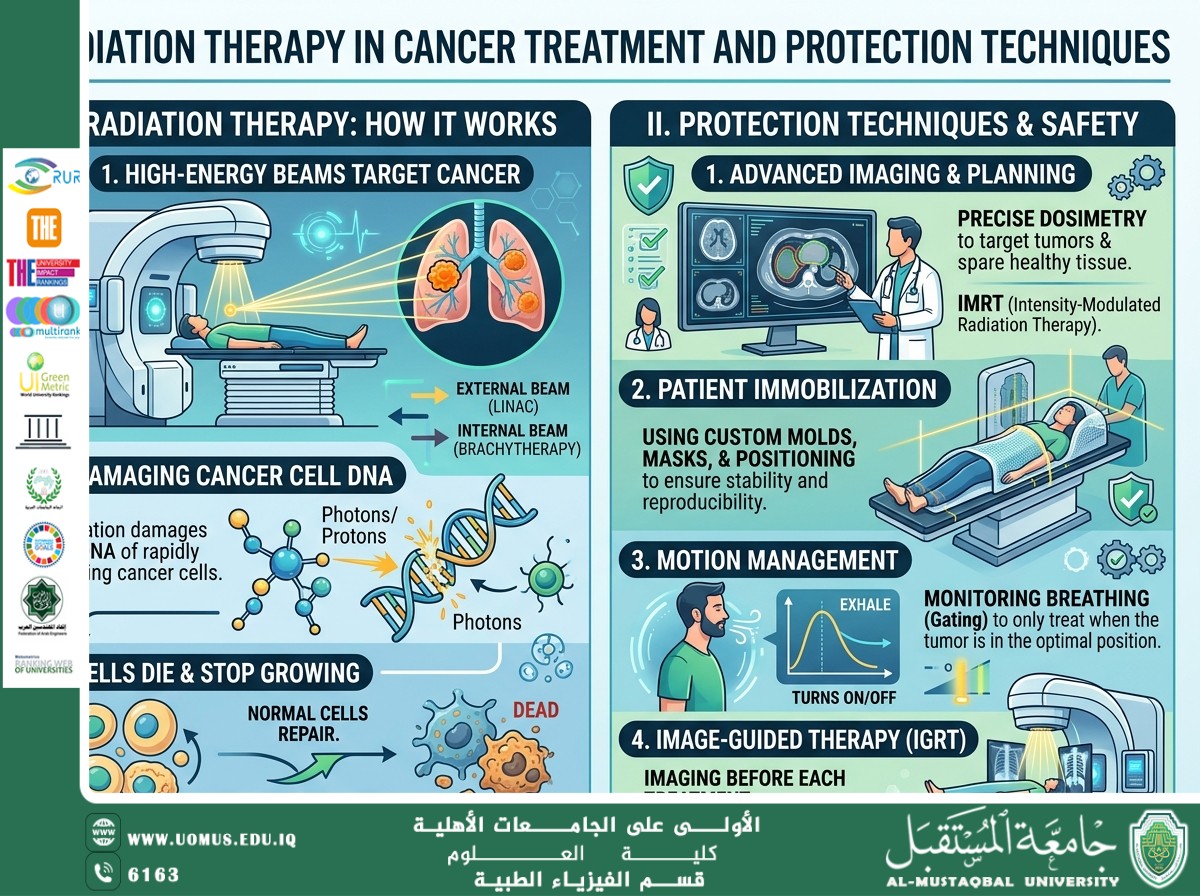
Radiation therapy works by delivering carefully calculated doses of ionizing radiation (such as X-rays or gamma rays) to the tumor. This radiation causes damage to the DNA of cancer cells, preventing them from dividing and proliferating. Cancer cells are generally more sensitive to radiation than normal cells, which allows for effective targeting.
Types of Radiation Therapy
Radiation therapy can be classified into several main types:
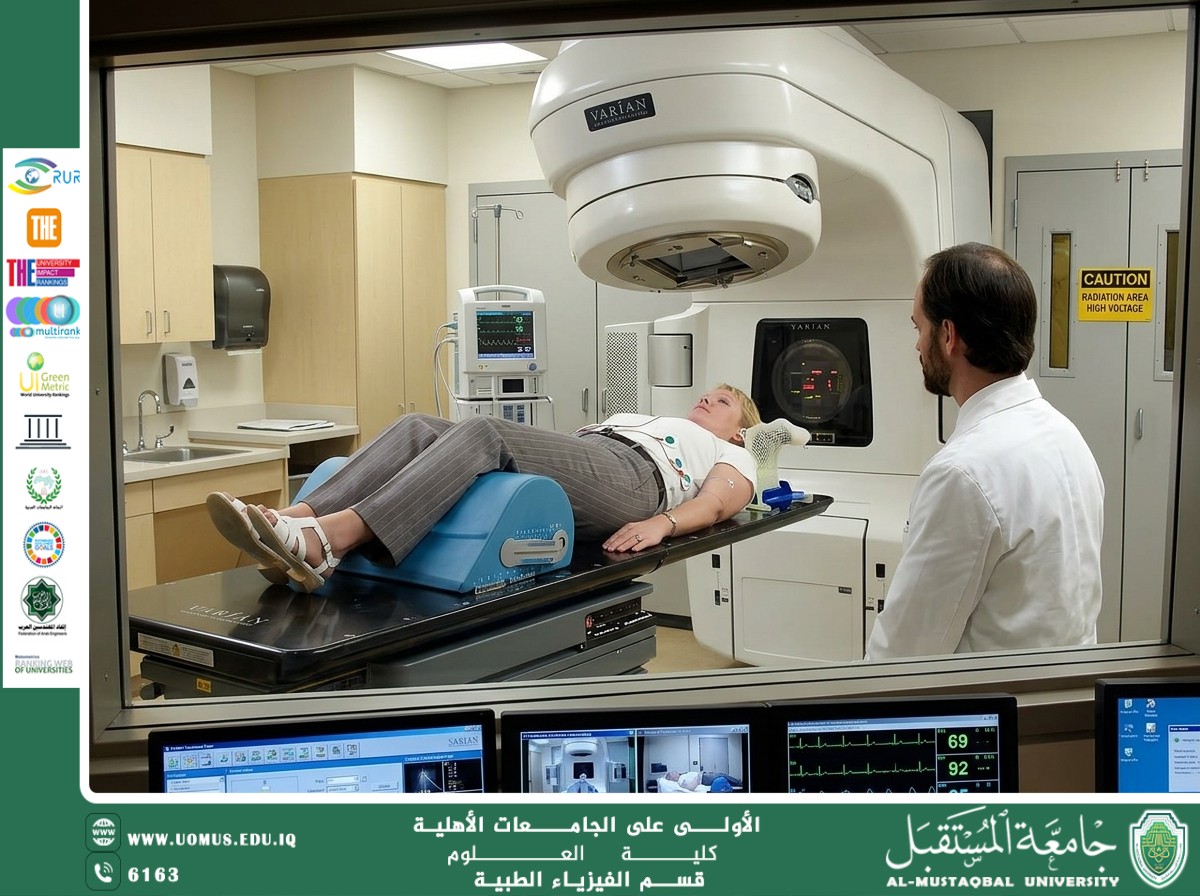
• External Beam Radiation Therapy (EBRT): Radiation is delivered from a machine outside the body and directed toward the tumor.
• Brachytherapy: A radioactive source is placed inside or near the tumor.
• Systemic Radiation Therapy: Radioactive substances are administered orally or via injection and circulate throughout the body.
Physical Challenges in Radiation Therapy
Medical physicists face several challenges, including:
• Determining the optimal dose that effectively destroys the tumor while minimizing damage to healthy tissues.
• Accurate dose distribution calculations within the body using advanced computational models and software.
• Managing organ motion, such as lung movement during breathing.
• Radiation scattering within tissues, which affects treatment accuracy.
Techniques for Improving Treatment Accuracy
To overcome these challenges, advanced techniques have been developed, such as:
• Image-Guided Radiation Therapy (IGRT) to enhance targeting precision.
• Intensity-Modulated Radiation Therapy (IMRT), allowing dose variation according to tumor shape.
• Proton Therapy, which provides higher precision and reduces dose to surrounding healthy tissues.
• Three-dimensional treatment planning (3D Planning) using CT and MRI imaging.
Radiation Protection Techniques
Radiation protection is a critical component of treatment and includes:
• Patient protection by minimizing dose to non-target tissues.
• Staff protection through shielding and radiation dose monitoring.
• Treatment room design using shielding materials such as lead and concrete.
• Application of radiation safety principles, including the ALARA principle.
Challenges and Future Directions
Key challenges include:
• Reducing long-term side effects.
• Improving targeting accuracy for small tumors.
Future directions involve:
• Integration of Artificial Intelligence (AI) in treatment planning.
• Development of more precise and faster treatment systems.
• Combining radiation therapy with advanced approaches such as immunotherapy.
Conclusion
Radiation therapy represents one of the most important tools in cancer management, combining precision and effectiveness. With advancements in medical physics, it has become possible to improve treatment outcomes while reducing associated risks. This enhances recovery rates, minimizes side effects, and highlights the importance of this field in supporting modern healthcare systems
"AL-Mustaqbal University is the first university in Iraq."