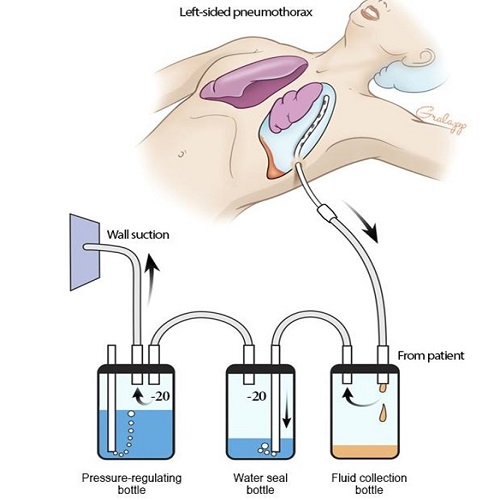
Chest tube
31/10/2024 Share :
A chest tube is a plastic tube that is used to drain fluid or air from the chest. Air or fluid (for example blood or pus) that collects in the space between the lungs and chest wall (the pleural space) can cause the lung to collapse. Chest tubes can be inserted at the end of a surgical procedure while a patient is still asleep from anesthesia or at the bedside using a local pain killer and some sedation. Chest tubes come in a variety of shapes and sizes. Depending on what they are needed for, they can range in diameter from as small as a shoelace to as large as a highlighter.<br /> <br />Chest tube indications<br />• Pneumothorax: Air in the pleural space caused by trauma, lung disease, invasive pulmonary procedure, forceful coughing, surgical complication, or may occur spontaneously<br />•To drain air, the chest tube is placed in anterior chest at the second or third intercostal space<br />• Hemothorax: Blood in the pleural space caused by blunt/penetrating trauma or a complication of chest surgery<br />•To drain fluid, the chest tube is placed at lung base<br />• Pleural effusion: Excessive fluid in the pleural space caused by pneumonia, left ventricular heart failure, pulmonary embolism, cancer, or complication of surgery<br />• Chylothorax: Accumulation of lymphatic fluid in the pleural space caused by chest trauma, tumor, surgery<br />• Empyema: Pus from an infection, such as pneumonia; must always be drained no matter how small amount<br />• Other considerations: Preventively after cardiac/pulmonary surgery to drain blood postoperatively and prevent cardiac tamponade; also used to instill fluids (chemotherapy, sclerosing agent)<br />Types of CDUs<br />• Chest drainage unit (CDU): Traditional chest drainage unit consists of a collection chamber, water seal chamber, suction control chamber; can drain large amounts of fluid or air<br />• Smaller/lighter portable CDU: Mechanical one-way valve instead of water seal chamber; good for patient who needs drainage only (not suction to re-expand lung), such as non-complicated pneumothorax<br /> <br />• Heimlich valve: Contains a one-way flutter valve; air drains out when patient exhales; keep collection device upright and vented to prevent air buildup<br />• Indwelling pleural catheter: Drains chronic pleural effusions; drains fluid only; can be done at home every 1 or 2 days or when short of breath <br /><br />Chest tube insertion<br />• Done in patient’s room, interventional radiology, or the operating room<br />• Local anesthetic; patient may feel pressure as tube is inserted<br />• Aseptic (sterile) procedure<br />• Patient’s breathing will be easier once lung is re-expanded<br />• Position patient for comfort depending on site to be inserted<br />• Tube will be anchored with a suture<br />• Insertion site will have an occlusive dressing applied<br />• Connections securely taped<br />• Chest X-ray to confirm position and lung re-expansion <br />Risks and complications<br />• Bleeding: Usually minor, but may require surgery if extensive<br />• Infection: Likelihood increases the longer the chest tube is in place<br />• Subcutaneous emphysema: Characterized by swelling in face, neck, and chest; crackles on palpation<br />• Lung trauma/Broncho pleural fistula: Rare, but patient will have signs and symptoms of respiratory distress, bloody chest tube drainage; tube will be left in place until healed<br />Nursing considerations<br />• Monitor vital signs<br />• Assess breath sounds bilaterally<br />• Assess the insertion site<br />• Encourage the patient to cough<br />• Make sure connections are taped securely<br />• Keep collection apparatus below the level of the patient’s chest<br />• Check water seal and suction control chambers frequently<br />• Assess drainage for color<br />• Measure drainage every 8 hours or more often depending on patient’s condition<br />• Report immediately bright red blood or red free-flowing drainage >70ml/hour<br />• Reposition patient frequently<br />Care of chest tube and drainage unit<br />• Tubing: Avoid loops, aggressive manipulation such as “stripping” or “milking”<br />• Patency: To maintain patency, try “gentle” hand over-hand squeezing of tubing and release<br />• Clamping: Avoid except when replacing CDU, locating air leak, or assessing when tube will be removed<br />Removing the chest tube<br />1- There’s little to no drainage<br />2- Air leak is gone<br />3- Patient is breathing normally without respiratory distress<br />4- Fluctuations in water seal chamber stopped<br />5- Chest X-ray shows lung re-expansion with no residual air or fluid<br />Procedure for chest tube removal<br />• Gather supplies and explain procedure to patient<br />• The clinician will remove the dressing and sutures<br />• During peak exhalation, the clinician will remove the chest tube in one quick movement<br />• Immediately apply a sterile gauze dressing containing petroleum to prevent air from entering pleural space<br />• Arrange for chest X-ray to confirm lung re-expansion<br />• Monitor patient’s respiratory status and SpO2 for 1-2 hours after removal.<br /><br />Done by : Noor Salah Mahdi<br />