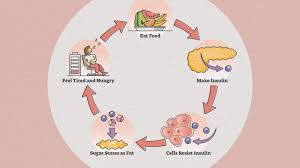
What is insulin resistance?
26/11/2024 Share :
Insulin resistance, also known as impaired insulin sensitivity, happens when cells in your muscles, fat and liver don’t respond as they should to insulin, a hormone your pancreas makes that’s essential for life and regulating blood glucose (sugar) levels. Insulin resistance can be temporary or chronic and is treatable in some cases.<br />Under normal circumstances, insulin functions in the following steps:<br />• Your body breaks down the food you eat into glucose (sugar), which is your body’s main source of energy.<br />• Glucose enters your bloodstream, which signals your pancreas to release insulin.<br />• Insulin helps glucose in your blood enter your muscle, fat and liver cells so they can use it for energy or store it for later use.<br />• When glucose enters your cells and the levels in your bloodstream decrease, it signals your pancreas to stop producing insulin.<br />For several reasons, your muscle, fat and liver cells can respond inappropriately to insulin, which means they can’t efficiently take up glucose from your blood or store it. This is insulin resistance. As a result, your pancreas makes more insulin to try to overcome your increasing blood glucose levels. This is called hyperinsulinemia.<br />As long as your pancreas can make enough insulin to overcome your cells’ weak response to insulin, your blood sugar levels will stay in a healthy range. If your cells become too resistant to insulin, it leads to elevated blood glucose levels (hyperglycemia), which, over time, leads to prediabetes and Type 2 diabetes.<br />In addition to Type 2 diabetes, insulin resistance is associated with several other conditions, including:<br />• Obesity.<br />• Cardiovascular disease.<br />• Nonalcoholic fatty liver disease.<br />• Metabolic syndrome.<br />• Polycystic ovary syndrome (PCOS).<br /><br /><br /><br /><br />What is the difference between insulin resistance and diabetes?<br />Anyone can develop insulin resistance — temporarily or chronically. Over time, chronic insulin resistance can lead to prediabetes and then Type 2 diabetes if it’s not treated or able to be treated.<br />Prediabetes happens when your blood glucose levels are higher than normal, but not high enough to be diagnosed as diabetes. Prediabetes usually occurs in people who already have some insulin resistance.<br />Prediabetes can lead to Type 2 diabetes (T2D), the most common type of diabetes. T2D happens when your pancreas doesn’t make enough insulin or your body doesn’t use insulin well (insulin resistance), resulting in high blood glucose levels.<br />Type 1 diabetes (T1D) happens when your body’s immune system attacks and destroys the insulin-producing cells in your pancreas for an unknown reason. T1D is an autoimmune and chronic disease, and people with T1D have to inject synthetic insulin to live and be healthy. While T1D is not caused by insulin resistance, people with T1D can experience levels of insulin resistance in which their cells don’t respond well to the insulin they inject.<br />Gestational diabetes is a temporary form of diabetes that can happen during pregnancy. It’s caused by insulin resistance that’s due to the hormones the placenta makes. Gestational diabetes goes away once you deliver your baby. Approximately 3% to 8% of all people who are pregnant people in the United States are diagnosed with gestational diabetes.<br />Healthcare providers often use a blood test called glycated hemoglobin (A1c) to diagnose diabetes. It shows your average blood sugar level for the past three months. In general:<br />• An A1c level below 5.7% is considered normal.<br />• An A1c level between 5.7% and 6.4% is considered prediabetes.<br />• An A1c level of 6.5% or higher on two separate tests indicates type 2 diabetes.<br /><br /><br /><br /><br /><br />Who does insulin resistance affect?<br />Insulin resistance can affect anyone — you don’t have to have diabetes — and it can be temporary (for example, using steroid medication for a brief period causes insulin resistance) or chronic. The two main factors that seem to contribute to insulin resistance are excess body fat, especially around your belly, and a lack of physical activity.<br />People who have prediabetes and Type 2 diabetes usually have some level of insulin resistance. People with Type 1 diabetes can also experience insulin resistance.<br />How does insulin resistance affect my body?<br />The development of insulin resistance typically increases insulin production (hyperinsulinemia) so your body can maintain healthy blood sugar levels. Elevated levels of insulin can result in weight gain, which, in turn, makes insulin resistance worse.<br />Hyperinsulinemia is also associated with the following conditions:<br />• Higher triglyceride levels.<br />• Hardening of the arteries (atherosclerosis).<br />• High blood pressure (hypertension).<br />Insulin resistance is also the main feature of metabolic syndrome, which is a set of features that link excess fat around the waist and insulin resistance to increased risk of cardiovascular disease, stroke and Type 2 diabetes.<br />Features of metabolic syndrome include:<br />• Elevated blood glucose levels.<br />• An elevated triglyceride level.<br />• Low levels of high-density lipoprotein (HDL) cholesterol.<br />• High blood pressure.<br />You don’t have to have all four of these features to have metabolic syndrome.<br /><br /><br /><br /><br /><br />Symptoms and Causes<br />What are the symptoms of insulin resistance?<br />If you have insulin resistance, but your pancreas can increase insulin production to keep your blood sugar levels in range, you won’t have any symptoms.<br />However, over time, insulin resistance can get worse, and the cells in your pancreas that make insulin can wear out. Eventually, your pancreas is no longer able to produce enough insulin to overcome the resistance, leading to elevated blood sugar (hyperglycemia), which does cause symptoms.<br />Symptoms of high blood sugar include:<br />• Increased thirst.<br />• Frequent urination (peeing).<br />• Increased hunger.<br />• Blurred vision.<br />• Headaches.<br />• Vaginal and skin infections.<br />• Slow-healing cuts and sores.<br />Many people have no symptoms of prediabetes, often for years. Prediabetes may be invisible until it develops into Type 2 diabetes. Some people with prediabetes may experience the following symptoms:<br />• Darkened skin in your armpit or back and sides of your neck, called acanthosis nigricans.<br />• Skin tags (small skin growths).<br />• Eye changes that can lead to diabetes-related retinopathy.<br />If you’re experiencing any of these symptoms, it’s important to see your healthcare provider.<br />What causes insulin resistance?<br />Scientists still have a lot to discover about how exactly insulin resistance develops. So far, they’ve identified several genes that make a person more or less likely to develop insulin resistance. In addition, older people are more prone to insulin resistance.<br />Several factors and conditions can cause varying degrees of insulin resistance. Scientists believe that excess body fat, especially around your belly, and physical inactivity are the two main contributing factors to insulin resistance.<br />Acquired causes of insulin resistance<br />Acquired causes, meaning you’re not born with the cause, of insulin resistance include:<br />• Excess body fat: Scientists believe obesity, especially excess fat in your belly and around your organs (visceral fat), is a primary cause of insulin resistance. A waist measurement of 40 inches or more for men and people assigned male at birth and 35 inches or more for women and people assigned female at birth is linked to insulin resistance. Studies have shown that belly fat makes hormones and other substances that can contribute to long-term inflammation in your body. This inflammation may play a role in insulin resistance<br />• Physical inactivity: Physical activity makes your body more sensitive to insulin and builds muscle that can absorb blood glucose. A lack of physical activity can have opposite effects and cause insulin resistance. In addition, a lack of physical activity and a sedentary lifestyle are associated with weight gain, which can also contribute to insulin resistance.<br />• Diet: A diet of highly processed, high-carbohydrate foods and saturated fats has been linked to insulin resistance. Your body digests highly processed, high-carbohydrate foods very quickly, which causes your blood sugar to spike. This puts extra stress on your pancreas to produce a lot of insulin, which, over time, can lead to insulin resistance.<br />• Certain medications: Certain medications can cause insulin resistance, including steroids, some blood pressure medications, certain HIV treatments <br /><br />Management and Treatment<br />How is insulin resistance treated?<br />Since not all factors that contribute to insulin resistance can be treated, such as genetic factors and age, lifestyle modifications are the primary treatment for insulin resistance. Lifestyle modifications include:<br />• Eating a healthy diet: Your healthcare provider or nutritionist may recommend avoiding eating excessive amounts of carbohydrates (which stimulate excess insulin production) and eating less unhealthy fat, sugar, red meats and processed starches. Instead, they’ll likely recommend eating a diet of whole foods that includes more vegetables, fruits, whole grains, fish and lean poultry.<br />• Physical activity: Getting regular amounts of moderate-intensity physical activity helps increase glucose energy usage and improve muscle insulin sensitivity. A single session of moderate-intensity exercise can increase glucose uptake by at least 40%.<br />• Losing excess weight: Your healthcare provider may recommend trying to lose excess weight to try treating insulin resistance. One study revealed that losing 7% of your excess weight can reduce the onset of Type 2 diabetes by 58%.<br />Over time, these lifestyle modifications can:<br />• Increase insulin sensitivity (reduce insulin resistance).<br />• Lower your blood glucose levels.<br />• Decrease blood pressure.<br />• Decrease triglyceride and LDL (“bad”) cholesterol levels.<br />• Raise HDL (“good”) cholesterol levels.<br />You may work with other healthcare providers, such as a nutritionist and endocrinologist, in addition to your regular doctor to come up with an individualized treatment plan that works best for you.<br /><br />د. رؤى نشأت