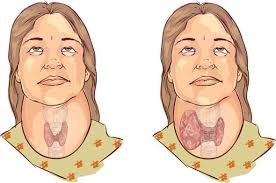
Endemic Goitre
27/11/2024 Share :
Endemic goitre, characterized by thyroid gland enlargement, is a prevalent public health issue primarily caused by iodine deficiency. It significantly impacts populations in areas where iodine intake is inadequate, particularly in mountainous and low-resource regions.<br /><br />Etiology and Pathophysiology<br /><br />The main cause of endemic goitre is insufficient dietary iodine, an essential element for thyroid hormone synthesis. Low iodine levels lead to reduced production of thyroxine (T4) and triiodothyronine (T3), stimulating increased thyroid-stimulating hormone (TSH) secretion, which promotes thyroid hypertrophy and hyperplasia. Secondary factors such as goitrogens in foods (e.g., cassava and millet) and genetic predispositions may exacerbate the condition.<br /><br />Epidemiology<br /><br />Endemic goitre affects approximately 30% of the global population, predominantly in regions with iodine-deficient soil, such as the Himalayas, Andes, and parts of sub-Saharan Africa. According to the World Health Organization (WHO), iodine deficiency disorders (IDDs) remain a leading cause of preventable intellectual disability worldwide.<br /><br />Clinical Manifestations<br /><br />The presentation ranges from asymptomatic thyroid enlargement to large, visible goitres causing compressive symptoms like dysphagia and dyspnea. Prolonged iodine deficiency can lead to hypothyroidism, developmental delays in children, and cretinism in severe cases.<br /><br />Diagnosis<br /><br />Endemic goitre is diagnosed through:<br />1. Clinical Examination: Thyroid size assessment<br />2. Urinary Iodine Testing: Measures iodine deficiency prevalence in a population.<br />3. Thyroid Function Tests: Evaluates TSH, T3, and T4 levels.<br /><br />Prevention and Management<br /><br />The cornerstone of prevention is universal salt iodization (USI), which has proven highly effective in reducing iodine deficiency globally. Other measures include dietary supplementation and public health education on iodine-rich foods (e.g., seafood, dairy).<br /><br />Treatment depends on severity:<br />• Mild Cases: Iodine supplementation or dietary adjustment.<br />• Severe Cases: Surgical resection for large goitres or hormone replacement therapy for hypothyroidism.<br /><br />Conclusion<br /><br />Endemic goitre remains a significant health challenge in iodine-deficient regions. While universal salt iodization has greatly reduced its prevalence, sustained public health efforts and monitoring are critical to achieving its eradication and preventing associated developmental and cognitive impairments.<br />م.د احمد تركي هاني فارس<br /><br />References<br />1. World Health Organization (WHO). “Iodine Deficiency Disorders.”<br />2. Zimmermann, M. B. (2009). “Iodine deficiency.” Endocrine Reviews.<br />3. Delange, F. (2001). “Iodine deficiency as a cause of brain damage.” Postgraduate Medical Journal.<br />4. UNICEF. “The State of the World’s Children: Maternal and Newborn Health.”