A scientific article by the lecturers, Assist.Prof.Dr. Munther Sameen Shukur / Lect. Mohaimen Sameer Aref / Lect. Ali Hadi Al-Husseini (Diabetic Retinopathy: Early Diagnosis and Treatment)
22/07/2025 Share :
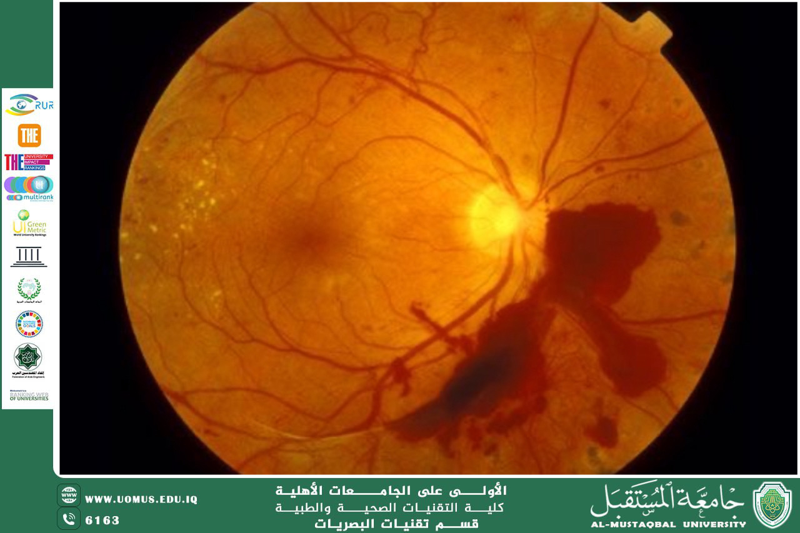
Diabetic retinopathy is a serious complication of diabetes that results from damage to the small blood vessels supplying the retina, caused by chronically elevated blood glucose levels. This damage can lead to fluid leakage or the growth of abnormal blood vessels, which may result in intraocular hemorrhage or retinal detachment—potentially leading to vision loss if left untreated.<br />The condition is classified into two main stages: non-proliferative diabetic retinopathy (NPDR), which involves early microvascular changes such as microaneurysms and macular edema and may initially be asymptomatic; and proliferative diabetic retinopathy (PDR), the more advanced stage characterized by the growth of abnormal new vessels, which can cause severe complications.<br />Early symptoms that patients may notice include blurred vision, floaters, reduced night vision, and difficulty distinguishing colors. However, symptoms often remain unnoticed until the disease progresses, making annual eye examinations essential for individuals with diabetes.<br />Diagnosis is typically conducted through dilated fundus examination, fluorescein angiography, and optical coherence tomography (OCT) to assess the presence of macular edema. Treatment strategies involve strict control of blood glucose, blood pressure, and lipid levels, in addition to laser photocoagulation, intravitreal injections of anti-VEGF agents, and vitrectomy surgery in advanced cases.<br />Prevention requires a strong commitment to a healthy lifestyle and regular screenings. Early detection and timely intervention are the key factors in preserving vision and preventing irreversible blindness.<br />