مقالة علمية للدكتورة سجا لطيف سلمان بعنوانThe Interrelationship Between Diabetes Mellitus and Thyroid Disorders
The Interrelationship Between Diabetes Mellitus and Thyroid Disorders
Diabetes mellitus (DM) and thyroid disorders are the most prevalent endocrine diseases worldwide. Their coexistence is more frequent than expected by chance and is associated with poor metabolic control and increased cardiovascular risk. Thyroid hormones regulate carbohydrate metabolism, insulin sensitivity, and lipid homeostasis, while diabetes alters thyroid hormone metabolism and pituitary regulation. This bidirectional relationship necessitates early detection and integrated management. This review summarizes current evidence regarding epidemiology, mechanisms, clinical implications, and screening strategies for patients with both disorders.
Diabetes mellitus affects over 537 million adults globally, while thyroid disorders affect more than 200 million individuals worldwide. Both conditions significantly impact metabolic processes and are associated with increased morbidity and mortality. Clinical studies demonstrate that patients with diabetes have a two- to three-fold higher prevalence of thyroid dysfunction compared with the general population. This relationship is particularly evident in patients with type 1 diabetes due to shared autoimmune mechanisms. Recognition of this endocrine interplay is essential for optimizing clinical outcomes.
The prevalence of thyroid dysfunction among patients with diabetes ranges from 10% to 15%, compared with 4–6% in the general population. Hypothyroidism is the most common abnormality.
• Type 1 DM: 20–30% develop autoimmune thyroid disease.
• Type 2 DM: 8–12% have subclinical hypothyroidism.
Women and elderly patients have a higher prevalence.
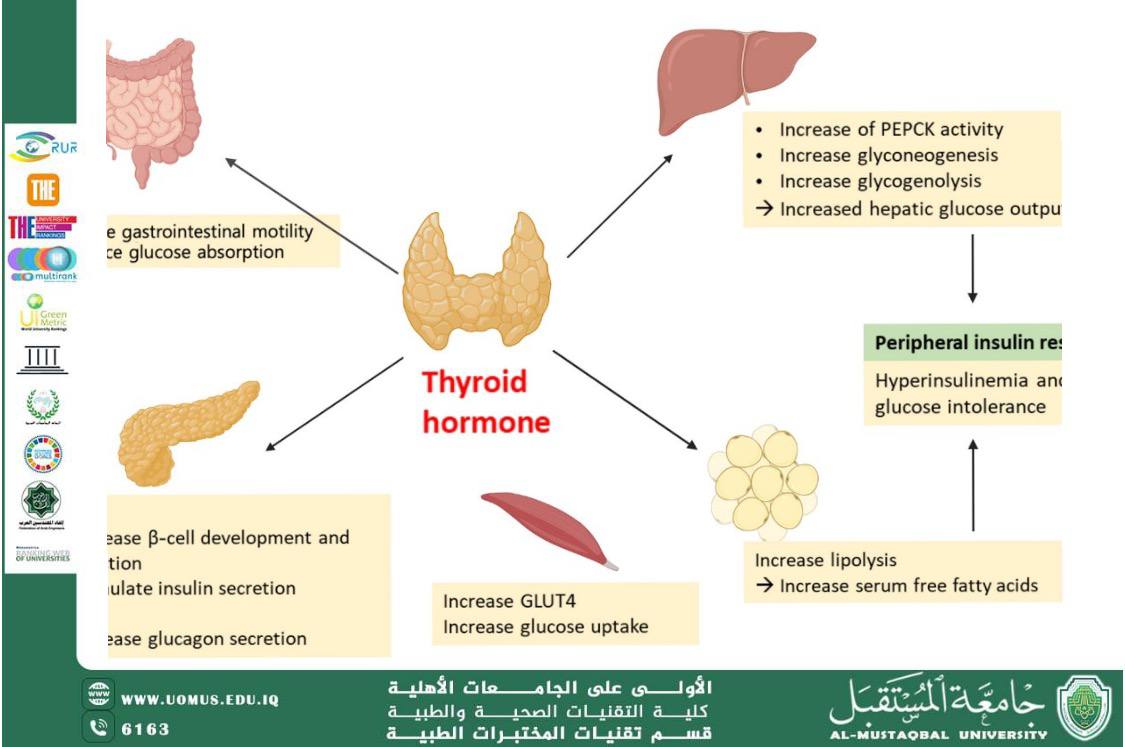
Effect of Thyroid Hormones on Glucose Metabolism
Thyroid hormones influence hepatic gluconeogenesis, intestinal glucose absorption, insulin secretion, and peripheral glucose uptake.
Thyroid State
Metabolic Effect
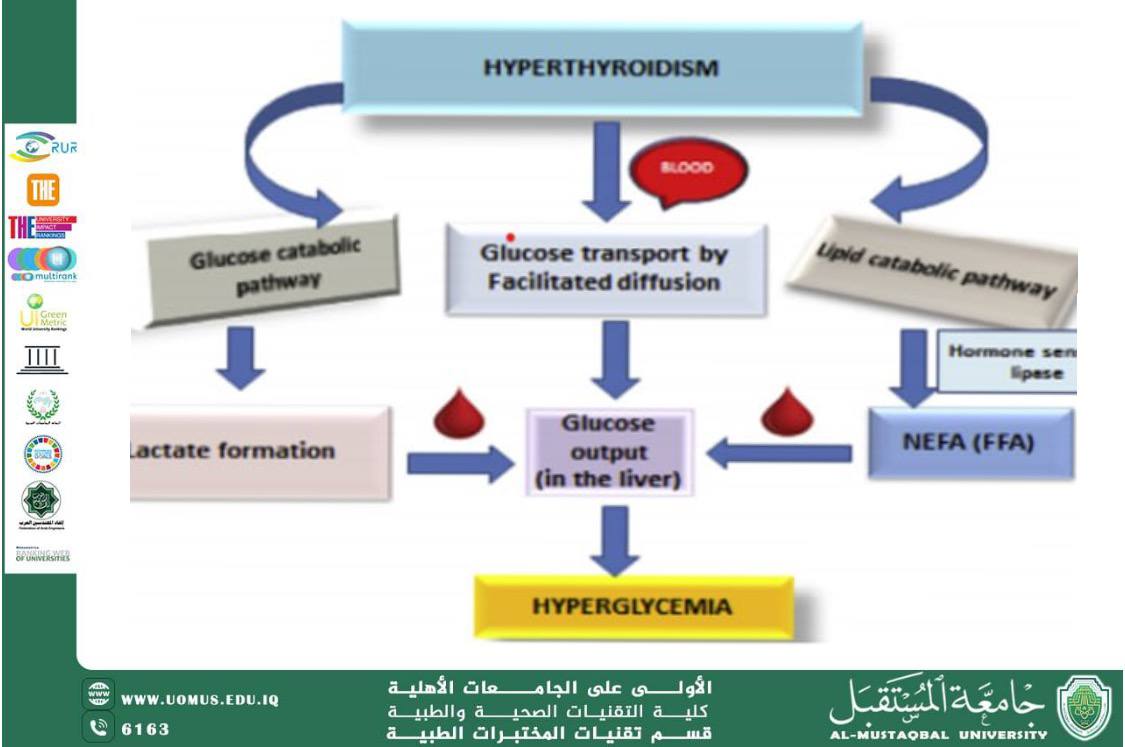
Hyperthyroidism
Increased hepatic glucose output, increased insulin resistance
Hypothyroidism
Reduced glucose absorption, decreased insulin clearance
Effect of Diabetes on Thyroid Function
Poor glycemic control reduces peripheral conversion of T4 to T3 and alters TSH secretion. Chronic hyperglycemia impairs hypothalamic–pituitary–thyroid axis activity.
Autoimmune Link
Type 1 diabetes and autoimmune thyroid diseases (Hashimoto’s thyroiditis, Graves’ disease) share genetic susceptibility (HLA-DR3, CTLA-4 polymorphisms), explaining their frequent coexistence.
Clinical Impact
Thyroid Disorder
Effect on Glycemic Control
Hyperthyroidism
Worsens hyperglycemia, increases insulin requirements
Hypothyroidism
Increases risk of hypoglycemia, decreases insulin requirements
Diagnostic Evaluation
Test
Purpose
TSH
Primary screening
Free T4, Free T3
Confirm thyroid status
Anti-TPO antibodies
Detect autoimmune disease
HbA1c, Fasting plasma glucose
Assess diabetes control
Management and Screening
Routine thyroid screening is recommended in diabetic patients, particularly those with type 1 DM. Integrated management improves glycemic control and reduces complications.
The bidirectional relationship between diabetes and thyroid disorders significantly influences metabolic control and cardiovascular risk. Early screening and combined treatment strategies are essential
جامعة المستقبل الجامعة الاولى في العراق
قسم تقنيات المختبرات الطبية الاول في التصنيف الوطني العراقي