Parkinson’s Disease: Pathophysiological Mechanisms and Emerging Therapeutic Perspectives
Parkinson’s disease is the second most common neurodegenerative disorder after Alzheimer’s disease. It is a chronic and progressive movement disorder that primarily results from the degeneration of dopamine-producing neurons in a region of the brain known as the Substantia Nigra. The loss of dopamine disrupts the transmission of neural signals responsible for coordinating movement.
2. Biological Mechanism (Pathophysiology)
Scientific studies indicate that a key pathological hallmark of Parkinson’s disease is the accumulation of a protein called Alpha‑synuclein.
These proteins aggregate to form microscopic clumps known as Lewy bodies within neurons.
The presence of these inclusions leads to cellular toxicity and gradual neuronal death, ultimately disrupting neural circuits involved in motor control and cognitive functions.
3. Clinical Symptoms
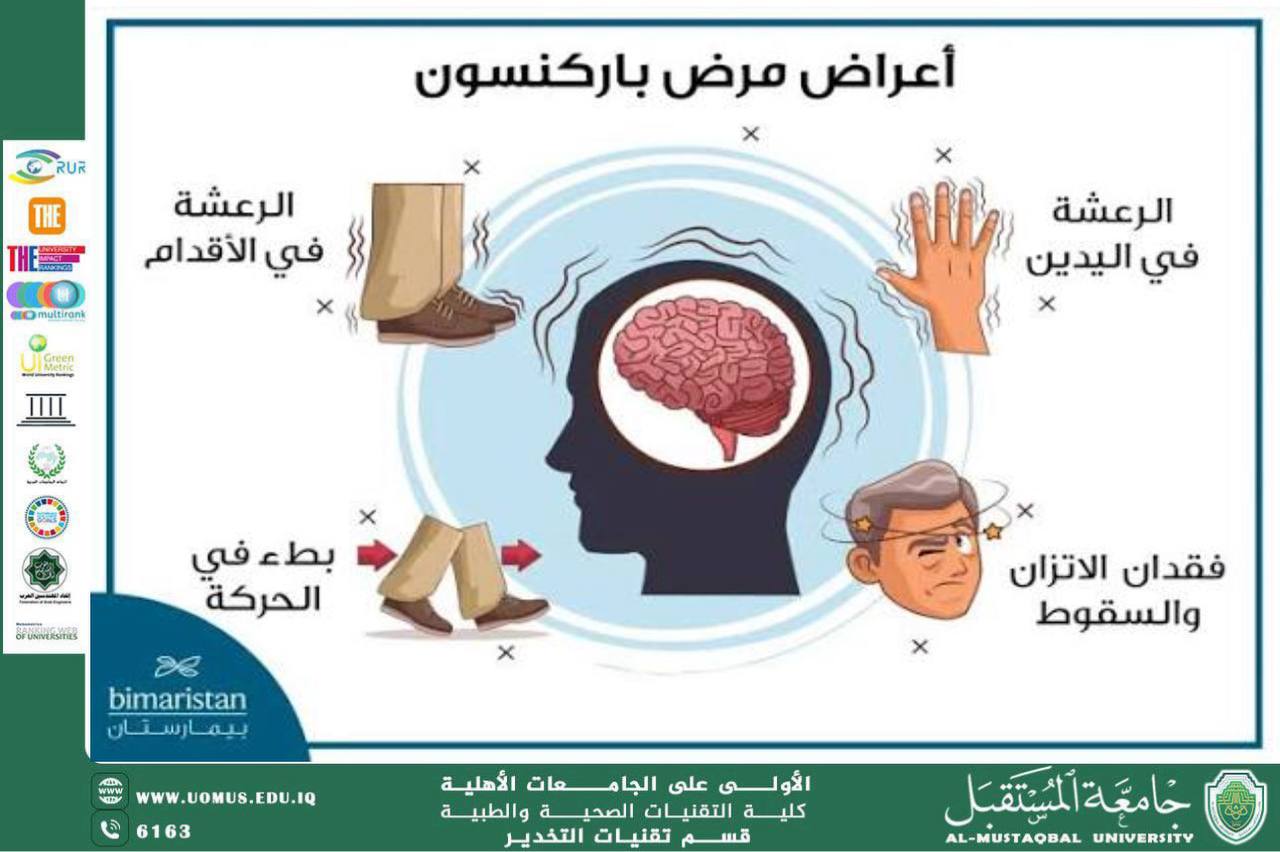
Symptoms are generally divided into two main categories:
• Motor symptoms: resting tremor, bradykinesia (slowness of movement), muscle rigidity, and postural instability.
• Non-motor symptoms: which may appear years before motor symptoms, including loss of smell, sleep disturbances, depression, and constipation.
4. Causes: Genetics and Environment
Current research suggests that the disease arises from a complex interaction between genetic and environmental factors:
• Genetic factors: Approximately 10–15% of cases are linked to specific genetic mutations, such as those affecting the LRRK2 and SNCA genes.
• Environmental factors: Exposure to certain pesticides or heavy metals may increase the risk of developing the disease, while some lifestyle-related factors may have a potential protective effect.
5. Recent Therapeutic Developments
Although there is currently no cure, significant advances have been made in treatment strategies:
• Pharmacological therapy: Levodopa remains the gold standard for replenishing dopamine levels.
• Surgical intervention: Deep Brain Stimulation (DBS), which involves implanting electrodes in specific brain regions to regulate abnormal electrical activity.
• Gene and cell therapies: Advanced clinical trials are underway using stem cells to replace damaged neurons, or viral vectors to modify defective genes.
• Biomarkers: Current research focuses on detecting the disease in the pre-symptomatic stage by measuring Alpha‑synuclein in cerebrospinal fluid or through advanced neuroimaging techniques.
6. Conclusion
Scientific research is increasingly moving toward personalized medicine, where treatment strategies are tailored according to each patient’s genetic profile. A deeper understanding of how Alpha‑synuclein spreads in the brain may open the door to developing vaccines or antibodies capable of halting disease progression in the near future.
Dr. Ahmed Neama
Al-Mustaqbal University
The First University in Iraq.