Irritable Bowel Syndrome (IBS)
20/01/2026 Share :
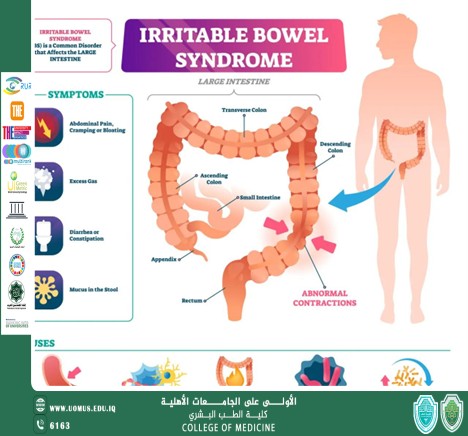
Irritable Bowel Syndrome (IBS) is a functional disorder of the large intestine characterized by recurrent abdominal pain associated with changes in bowel habits (diarrhea, constipation, or both), without any detectable organic cause on routine investigations.
Pathogenesis
IBS results from the interaction of several factors, mainly:
Increased sensitivity of the colon to pain and distension
Abnormal intestinal motility (either accelerated or slowed)
Disturbance in the brain–gut axis communication
Psychological factors such as stress, anxiety, and depression
Imbalance in gut flora (beneficial bacteria)
Sometimes occurs after previous intestinal infections
Causes and Triggering Factors
Psychological stress and daily life pressures
Certain foods (fatty foods, legumes, caffeine, spicy foods)
Changes in daily routine or travel
Sleep disturbances
Hormonal changes (especially in women)
Symptoms
Symptoms vary among individuals. Common manifestations include:
Abdominal pain or cramps, often relieved after defecation
Bloating and gas
Diarrhea or constipation, or alternating between both
Sensation of incomplete bowel evacuation
Mucus in the stool
IBS is usually NOT associated with:
Rectal bleeding
n
Weight loss
Anemia
(If any of these occur, further medical evaluation is required.)
Clinical Types
IBS-D: Diarrhea predominant
IBS-C: Constipation predominant
IBS-M: Mixed type
IBS-U: Undetermined type
Diagnosis
Diagnosis is based on:
Clinical history (Rome IV Criteria)
Simple investigations to exclude organic diseases when alarm features are present
❗ Colonoscopy is usually not required unless warning signs exist.
Treatment
1. Reassurance and Education
Explaining that IBS is a functional disorder
Emphasizing that it is not dangerous and does not lead to cancer
2. Lifestyle Modification
Stress and anxiety reduction
Regular sleep
Physical exercise
3. Dietary Management
Avoid foods that trigger symptoms
Increase intake of soluble fiber
4. Medical Treatment (according to symptoms)
Antispasmodics (e.g., Mebeverine)
Medications for diarrhea or constipation
Probiotics
Low-dose antidepressants when needed
5. Psychological Therapy (if required)
Cognitive Behavioral Therapy (CBT)
Relaxation techniques
Conclusion
Irritable Bowel Syndrome is a chronic functional disorder that is not dangerous but requires good understanding and cooperation between the doctor and patient. Lifestyle and dietary modifications play a key role in controlling symptoms and improving quality of life.