Scientific Article on Glucocorticoid Therapy – ADA 2026
Introduction
The use of glucocorticoid therapy is common in clinical practice for the management of many medical conditions. However, its association with the development of hyperglycemia represents a significant challenge, particularly among hospitalized patients, whether or not they have preexisting diabetes. According to the American Diabetes Association (ADA) Guidelines 2026, effective management of glucocorticoid-induced hyperglycemia requires an understanding of glycemic patterns, selection of appropriate treatment strategies, and continuous monitoring to ensure patient safety and reduce complications.
Glucocorticoid-Induced Hyperglycemia
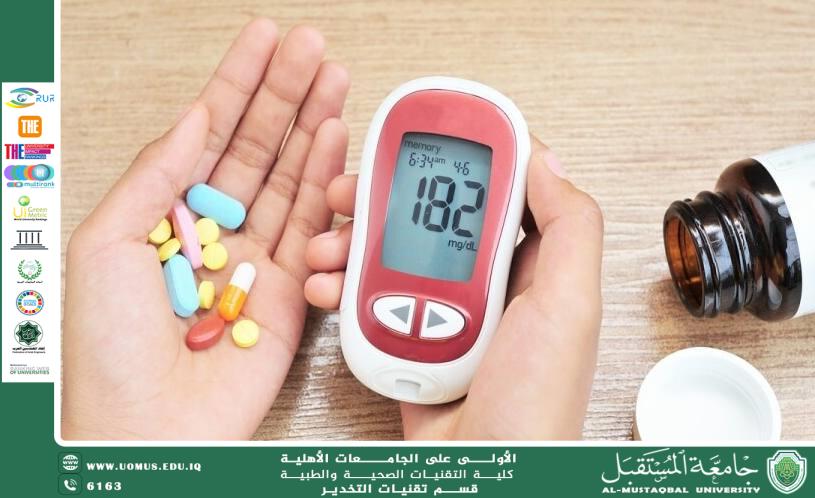
Glucocorticoids are widely used in hospitals, with approximately 10–15% of hospitalized patients receiving these medications. The risk of developing hyperglycemia is high, affecting about 56–86% of patients. Hyperglycemia may occur in patients with or without a prior diagnosis of diabetes. The severity and pattern of glucose elevation depend on several factors, including the type of steroid used, the dose administered, and the duration of action.
Typical Glycemic Pattern (Intermediate-Acting Steroids)
When intermediate-acting steroids such as prednisone or prednisolone are administered in the morning, fasting glucose levels are usually normal or mildly elevated. Blood glucose levels tend to rise during the afternoon, with peak hyperglycemia occurring in the evening. This pattern is more pronounced in patients with type 2 diabetes.
Insulin Strategies During Steroid Therapy
Intermediate-Acting Steroids
The combination of NPH insulin with prednisone or prednisolone is considered a preferred and practical option. The peak action of NPH insulin occurs after 4–6 hours, which corresponds well with the pharmacologic effect of the steroid. NPH insulin should be administered concurrently with the steroid dose and may be added to a basal–bolus insulin regimen or oral glucose-lowering agents, depending on the type of diabetes and prior treatment.
Long-Acting or Continuous Steroids
Steroids such as dexamethasone or multidose/continuous regimens often require the use of long-acting basal insulin. The primary goal in these cases is to achieve adequate fasting glucose control.
High-Dose Steroids
High-dose glucocorticoid therapy often necessitates increasing prandial and correction insulin doses by 40–60% or more, in addition to basal insulin. Increasing the insulin-to-steroid ratio may improve time-in-range glucose control but also increases the risk of hypoglycemia.
Monitoring and Adjustment
Effective management requires daily adjustment of insulin doses and frequent point-of-care blood glucose monitoring. These measures are essential to minimize the risks of hypoglycemia and steroid-induced hyperglycemia.
Conclusion
According to ADA 2026 guidelines, effective management of glucocorticoid-induced hyperglycemia relies on individualized patient assessment, consideration of the type and dose of glucocorticoid therapy, appropriate insulin strategy selection, and continuous glucose monitoring. This comprehensive approach contributes to reducing complications, improving clinical outcomes, and ensuring patient safety.
Dr Miaad Adnan
Al-Mustaqbal University
The First University in Iraq