A Scientific Article by Dr. Haider Haleem Saeed titled: Bacterial Joint Infection: Diagnosis, Treatment, and Prevention
1. Introduction
Bacterial joint infection, clinically known as septic arthritis, is a serious medical condition that occurs when bacteria enter a joint, leading to inflammation, pain, and potential joint destruction. Early diagnosis and treatment are essential to prevent permanent damage and systemic complications.
2. Epidemiology
Septic arthritis affects all age groups, but it is more common in:
• Older adults
• Individuals with weakened immune systems
• Patients with pre-existing joint diseases (e.g., rheumatoid arthritis)
• People with prosthetic joints
The incidence ranges from 2 to 10 cases per 100,000 people annually in developed countries, with higher rates in certain high-risk populations.
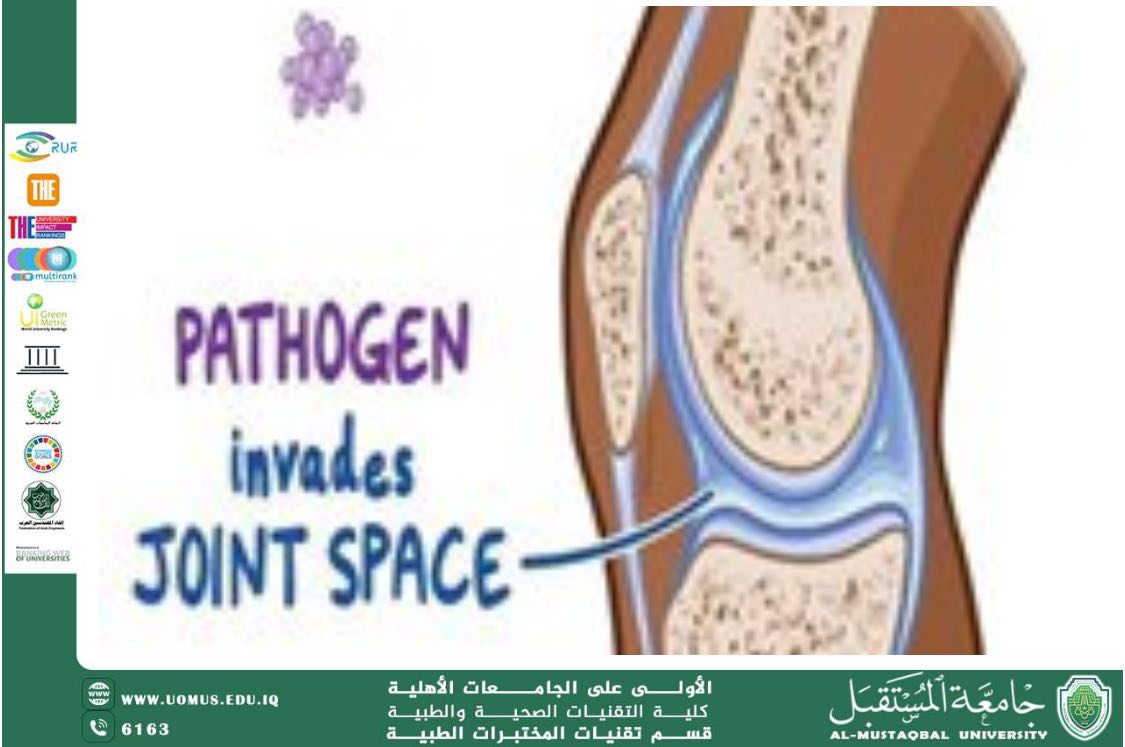
3. Pathogenesis – How Bacteria Infect Joints
Bacteria can reach the joint through several routes:
1. Hematogenous spread: Bacteria travel through the bloodstream from another site in the body (e.g., skin or urinary tract) and settle in the synovial membrane.
2. Direct inoculation: Through trauma, surgery, injections, or penetrating injuries.
3. Contiguous spread: From nearby infected tissues, such as osteomyelitis.
Once bacteria invade the joint:
• Synovial inflammation occurs.
• White blood cells, especially neutrophils, enter the joint and release enzymes and cytokines.
• These enzymes can rapidly damage cartilage and bone.
4. Common Causative Organisms
• Staphylococcus aureus: most common overall
• Streptococcus species: common in children and adults
• Neisseria gonorrhoeae: in sexually active adults
• Gram-negative bacilli: in older adults and immunocompromised patients
• Rare pathogens: after surgery or in patients with prosthetic joints
5. Clinical Presentation
Patients typically present with:
• Sudden onset joint pain
• Swelling and warmth
• Limited range of motion
• Fever and general malaise
Large joints such as the knee, hip, shoulder, and ankle are often affected.
6. Diagnosis
6.1 Physical Examination
• Tenderness over the joint
• Redness
• Pain on movement
6.2 Laboratory Tests
• Elevated white blood cell count
• Increased inflammatory markers (CRP, ESR)
6.3 Synovial Fluid Analysis
Joint aspiration is the gold standard for diagnosis:
• Appearance: cloudy and purulent
• White blood cell count: typically >50,000 cells/mm³
• Gram stain and culture identify the causative bacteria
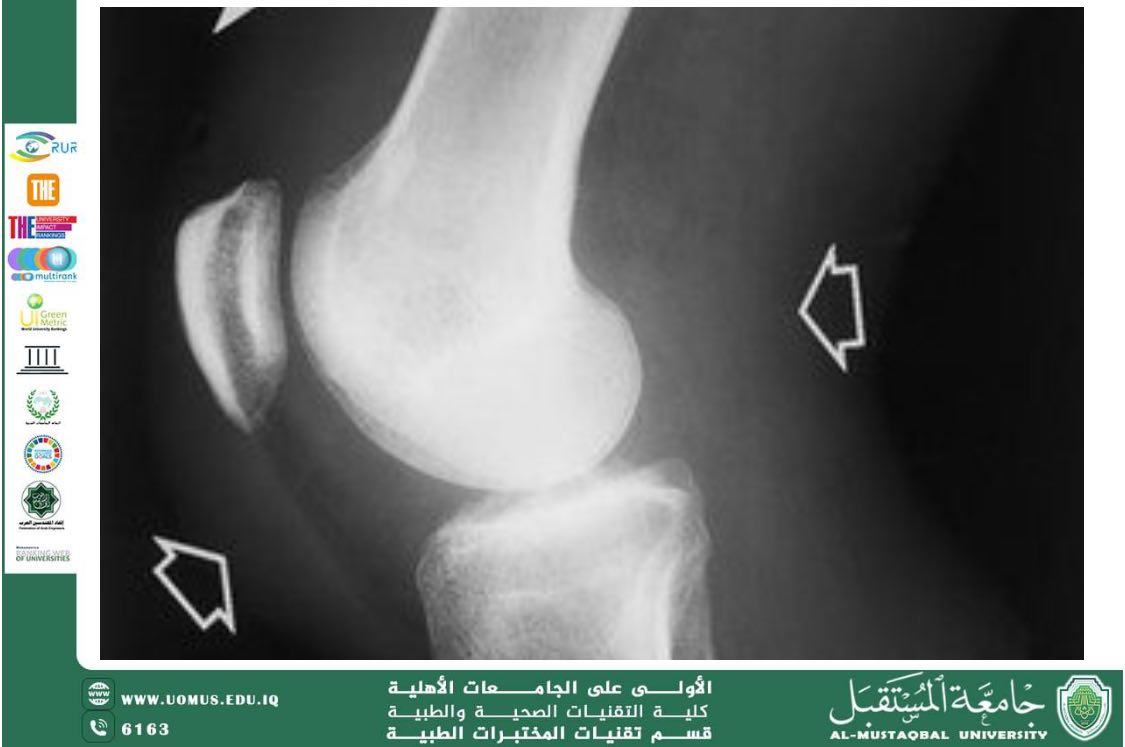
6.4 Imaging
• X-rays: may show joint space changes
• Ultrasound or MRI: useful for early detection
7. Treatment
Treatment usually includes:
7.1 Antibiotic Therapy
• Initial empiric broad-spectrum antibiotics
• Adjusted according to culture results
• Typical duration: 2–6 weeks
7.2 Joint Drainage
• Needle aspiration
• Repeated aspiration or surgical washout, especially in large joints
7.3 Supportive Care
• Pain management
• Physical therapy to maintain joint function after infection control
8. Complications
If treatment is delayed or absent:
• Joint destruction
• Osteomyelitis
• Sepsis
• Chronic pain and reduced mobility
9. Prevention
• Prompt treatment of bacteremia and skin infections
• Use of sterile techniques during joint procedures
• Vaccination for at-risk individuals (e.g., pneumococcal vaccine)
10. Conclusion
Bacterial joint infection is a medical emergency. Early recognition, accurate diagnosis, and aggressive treatment are essential to preserve joint integrity and prevent life-threatening complications.
Al-Mustaqbal University is the first university in Iraq
Department of Medical Laboratory Techniques – First in the Iraqi National Ranking.