Neglect of Vitamin D3 Assessment and Its Clinical Implications
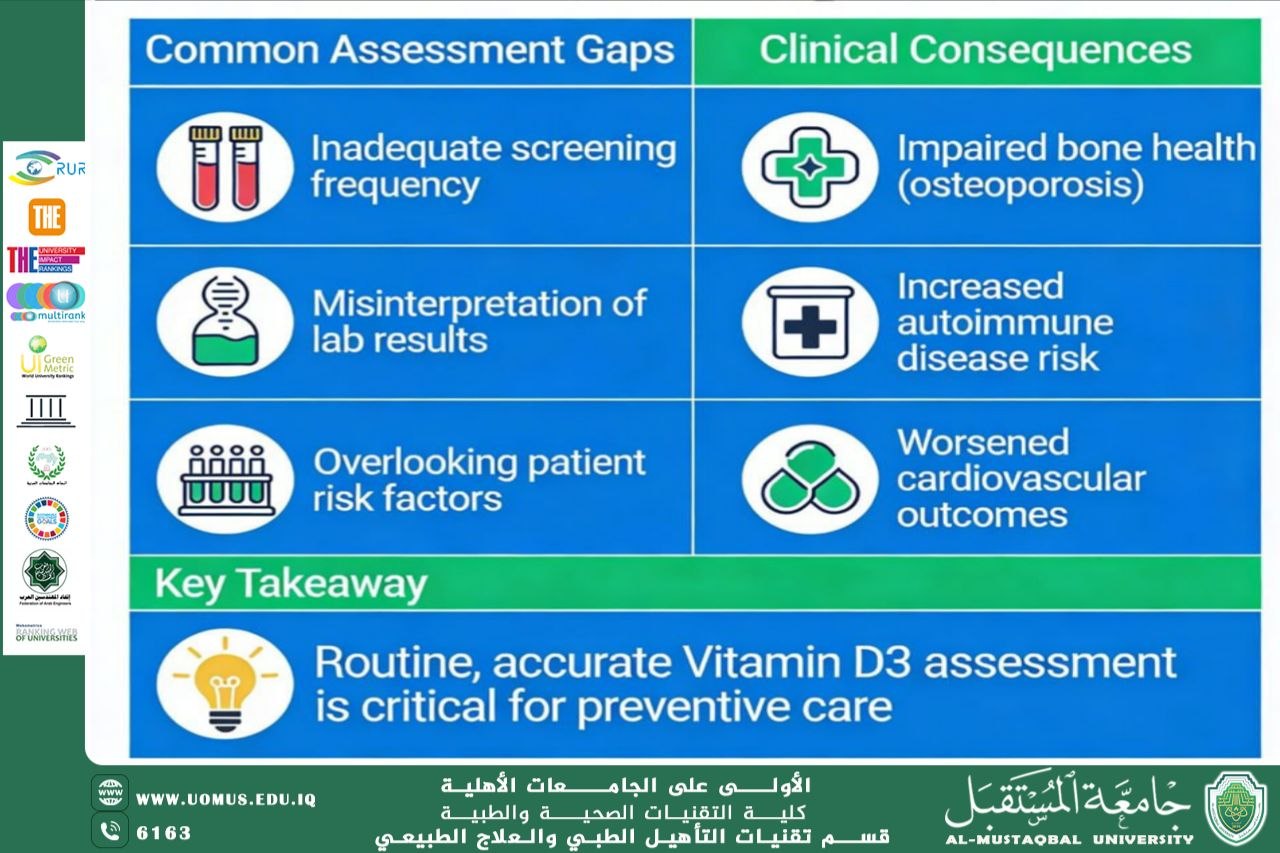
Vitamin D3 (cholecalciferol) is a critical secosteroid hormone involved in calcium–phosphate homeostasis, skeletal metabolism, and immunomodulatory functions. Despite its well-documented clinical relevance, assessment of vitamin D status is frequently underutilized in routine medical practice. Neglecting serum vitamin D3 evaluation may result in prolonged, unrecognized deficiency, contributing to a wide spectrum of musculoskeletal and systemic disorders. This article highlights the etiological factors underlying the neglect of vitamin D3 testing, its clinical consequences, and the necessity of systematic screening in high-risk populations.Vitamin D3 is synthesized endogenously in the skin upon exposure to ultraviolet B (UVB) radiation and undergoes subsequent hepatic and renal hydroxylation to form its biologically active metabolite, 1,25-dihydroxyvitamin D (calcitriol). This hormone exerts pleiotropic effects, particularly in bone mineralization, neuromuscular function, and immune regulation. Despite the high global prevalence of hypovitaminosis D, laboratory assessment of vitamin D status remains inconsistently performed, even in susceptible populations.The underassessment of vitamin D3 levels is multifactorial. Contributing factors include insufficient awareness among healthcare professionals, reliance on clinical presentation rather than biochemical confirmation, and the misconception that adequate sunlight exposure eliminates the risk of deficiency. Furthermore, the early manifestations of vitamin D deficiency are often subtle and non-specific, such as chronic fatigue, myalgia, and proximal muscle weakness, leading to misdiagnosis or clinical oversight. Prolonged vitamin D3 deficiency is strongly associated with impaired calcium absorption, secondary hyperparathyroidism, osteomalacia, osteoporosis, and an increased risk of fragility fractures. In pediatric populations, deficiency may result in rickets and growth retardation. Emerging clinical evidence also implicates vitamin D deficiency in immune dysregulation, increased susceptibility to infectious diseases, cardiovascular morbidity, insulin resistance, and neuropsychiatric disorders, including depressive syndromes. Serum 25-hydroxyvitamin D [25(OH)D] concentration is the most reliable biomarker for evaluating vitamin D status. Early identification of deficiency facilitates timely therapeutic intervention through targeted supplementation and lifestyle modification. Routine screening is particularly warranted in high-risk groups, including elderly individuals, pregnant and lactating women, patients with chronic kidney disease, malabsorption syndromes, and individuals with limited sun exposure. Neglecting vitamin D3 assessment constitutes a significant yet preventable clinical oversight with far-reaching health implications. Integrating vitamin D evaluation into standard diagnostic protocols and enhancing clinician awareness are essential for reducing the burden of vitamin D–related disorders. Systematic screening and evidence-based management strategies can substantially improve patient outcomes and overall public health.
Al-Mustaqbal University, the first university in Iraq.